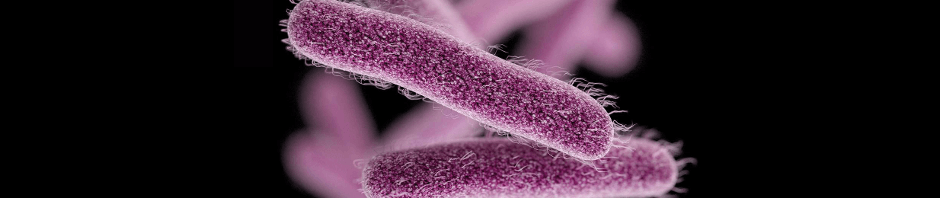
I came across a book called Brain Maker, which led me down the rabbit hole of gut bacteria. The author, David Perlmutter, and many other doctors, scientists, and researchers have found evidence of the profound impact our “belly bugs” have on our health. So profound that I decided to spread the word and give the following presentation.
I came across a book called Brain Maker, which led me down the rabbit hole of gut bacteria. The author, David Perlmutter, and many other doctors, scientists, and researchers have found evidence of the profound impact our “belly bugs” have on our health. So profound that I decided to spread the word and give the following presentation.
You’ve heard of the saying “butterflies in the stomach”. When we think of this, we think about things going on in our world – stresses or falling in love – and how our brain reacts to those things and makes our stomach feel wobbly.
 But it’s actually a two-way street, and it’s more of a two way street than many of us realize. There is a giant nerve called the Vagus nerve, the name Vagus coming from the same root word as vagabond, meaning to wander, because this nerve wanders from your brainstem to your abdomen, and travels all through your gastrointestinal tract in the process.
But it’s actually a two-way street, and it’s more of a two way street than many of us realize. There is a giant nerve called the Vagus nerve, the name Vagus coming from the same root word as vagabond, meaning to wander, because this nerve wanders from your brainstem to your abdomen, and travels all through your gastrointestinal tract in the process.
Your belly bugs send signals through this nerve up to your brain, and to other cells, and to organelles in cells. Some of the gut microbes release chemical messengers just like neurons do, so they speak to the brain in its own language, just like brain cells. The central nervous system, your brain and spinal cord, is created from the same tissue as the enteric nervous system, which governs your gastrointestinal tract. There are so many neurons in the gut that scientists have referred to it as your second brain.
 Your belly bugs regulate muscles, they control immune cells, and they make substances the body needs. For example, 80-90% of the serotonin produced in your body is produced by the gut. Serotonin is one of the S’s in SSRI, the category of antidepressants that Prozac falls into. It’s a “happiness” neurotransmitter. Depression and gut bacteria could be a talk all on their own.
Your belly bugs regulate muscles, they control immune cells, and they make substances the body needs. For example, 80-90% of the serotonin produced in your body is produced by the gut. Serotonin is one of the S’s in SSRI, the category of antidepressants that Prozac falls into. It’s a “happiness” neurotransmitter. Depression and gut bacteria could be a talk all on their own.
Belly bugs include bacteria, eukaryotic parasites, protozoa, and yeasts, which, together, are called the microbiome. Ed Yong, in his book, I Contain Multitudes, states, “about half of your cells are not human — enough to make you wonder what you mean by ‘you’.”
To keep things succinct, though, I’m going to focus on the bacteria inside of you, and their role in healthy brain function and prevention of disease.
Gut bacteria, en masse, weighs about the same as your brain, which is roughly 3 – 4 pounds. And about half of the weight in our feces is from bacteria. Half of the weight. In our poop. Bacteria. That’s a lot of bacteria in us.
 I think it’s exciting that we still don’t know a lot about these tiny organisms. It seems odd, given all the stuff we do know, all our technological advances in medicine and science. And our bodies. We’ve had these bodies since Homo sapiens came on the scene. And yet these bacteria, which play a HUGE role in our health, and are a big part of us, are still a mystery. Scientists are starting to figure it out now, and I think there’s going to be an explosion of information coming out in this area.
I think it’s exciting that we still don’t know a lot about these tiny organisms. It seems odd, given all the stuff we do know, all our technological advances in medicine and science. And our bodies. We’ve had these bodies since Homo sapiens came on the scene. And yet these bacteria, which play a HUGE role in our health, and are a big part of us, are still a mystery. Scientists are starting to figure it out now, and I think there’s going to be an explosion of information coming out in this area.
What we do know now, is that these “belly bugs” affect every organ in the human body. They affect cognitive function, digestion, breathing, the beating of your heart, and more. And while we don’t know what the ideal amount of each species living inside of us is, we do know that, just like with your stock portfolio, diversity is critical. And if certain ratios of this bacteria to that bacteria get out of whack, you have a problem.
For now, I’m going to highlight the top three ways that belly bugs affect brain health.
- They help control inflammation.
- They help prevent gut permeability.
- They produce important substances.
Perhaps one of the biggest impacts the microbiome has on the body’s health is its ability to regulate inflammatory reactions. You’ve probably heard of the “fight or flight” response, the nervous system’s automatic reaction to danger. Basically, when a threat is perceived, the body sends out an immune response to the affected site, and this results in swelling, heat, and redness, which we know of as inflammation. The problem is that the body can’t distinguish between actual threats and perceived threats, and when we are stressed, or our brain is being stressfully over-active, inflammation persists through deep systemic pathways inside our bodies, and this leads to illness.
Inflammatory markers, called cytokines, are one way that scientists track inflammation. Cytokines are proteins sent out by immune cells when the fight or flight reaction is triggered by a perceived threat. There are different kinds of cytokines, but one of the ones most talked about is TNF-alpha. TNF-alpha appears in abundance in a multitude of disease states.
The balance and diversity of gut bacteria regulates how much inflammation occurs within the body. Genetics play a role, too. But you can think of your gut bugs as helpful minions that boost your good gene activity, and inhibit the bad. Healthy levels of a variety of good bacteria limit the production of inflammatory chemicals in the body and the brain.
the production of inflammatory chemicals in the body and the brain.
Inflammation is the basis for many degenerative conditions in the human body. Click here to read more.
Inflammation in the brain is the foundation of Alzheimer’s disease. Inflammation and elevated blood glucose levels – elevated meaning at a less than diabetic level – go hand in hand. Out of control blood glucose in the body is a major cause of internal inflammation, and poor blood sugar control is highly linked with Alzheimer’s, so much so that some scientists refer to Alzheimer’s as Type III Diabetes.
When there is too much sugar in the blood stream, not only does that excess sugar stir up inflammation in the blood stream, but sugar molecules also combine with proteins and some fats to make Advanced Glycation Endproducts, AGEs. AGEs in the brain contribute to the degeneration of brain tissue, causing things like dementia and Alzheimer’s.
 Numerous studies showed that people with Type II diabetes also suffered from bacterial imbalances in the gut. Dysbiosis. Their bodies can’t transport glucose successfully from the blood stream into their cells. They’re under metabolic stress. And gut bacteria are needed to make byproducts that help maintain the health of the cells in the digestive system, for glucose control and more.
Numerous studies showed that people with Type II diabetes also suffered from bacterial imbalances in the gut. Dysbiosis. Their bodies can’t transport glucose successfully from the blood stream into their cells. They’re under metabolic stress. And gut bacteria are needed to make byproducts that help maintain the health of the cells in the digestive system, for glucose control and more.
There was a study done in China which showed why supplements work better on some people than others for controlling blood glucose levels. It has to do with your gut bugs. When you take a supplement for blood glucose control, such as chromium or berberine, the substance doesn’t go straight to the brain. It goes to your gut. Your gut bugs make use of these supplements first, so that they can have a positive effect on your health.
So if you have a healthy microbiome, your gut bugs will be better equipped to help you process glucose effectively, and control inflammatory responses. On the other hand, if you alter your microbiota, you may be paving the way for diabetes and the proliferation of AGEs in the brain, increasing the risk of Alzheimer’s and other degenerative brain ailments.
 The second major way that gut bacteria reduce your risk of brain disease is by reinforcing the intestinal wall’s integrity and preventing gut permeability. The gastrointestinal tract allows nutrients into your body so that your body can process them and then use them. The GI tract is also supposed to keep certain pathogens trapped in the gut. This GI tract has a thin mucous membrane made up of a single layer of epithelial cells. In between the cells are what are called tight junctions. Certain things, including an imbalance of gut bacteria, have been found to weaken these tight junctions. Compromised tight junctions allow various proteins, toxins, and other substances which should be kept in the gut to escape through the gut wall and challenge the immune system. This scenario turns on an immune response, and you get your inflammation.
The second major way that gut bacteria reduce your risk of brain disease is by reinforcing the intestinal wall’s integrity and preventing gut permeability. The gastrointestinal tract allows nutrients into your body so that your body can process them and then use them. The GI tract is also supposed to keep certain pathogens trapped in the gut. This GI tract has a thin mucous membrane made up of a single layer of epithelial cells. In between the cells are what are called tight junctions. Certain things, including an imbalance of gut bacteria, have been found to weaken these tight junctions. Compromised tight junctions allow various proteins, toxins, and other substances which should be kept in the gut to escape through the gut wall and challenge the immune system. This scenario turns on an immune response, and you get your inflammation.
A common substance that leaks through the gut and into the bloodstream and the brain is something called LPS, lipopolysaccharide. This is a fatty sugar compound that’s found on the outside of certain bacteria. It’s sort of like their “super skin” because it helps them to survive  in bile. But this LPS is not super in the bloodstream and brain. And lots of it is found in the brains of people who have Alzheimer’s, dementia, depression, and all sorts of other diseases, including psoriasis, and even autism.
in bile. But this LPS is not super in the bloodstream and brain. And lots of it is found in the brains of people who have Alzheimer’s, dementia, depression, and all sorts of other diseases, including psoriasis, and even autism.
You’ve probably heard of the blood-brain barrier. The physiology is a similar. There’s a lining around the brain that’s designed to regulate what gets in and out of the brain from the blood stream. What’s interesting is that people who have leaky gut syndrome often have leaky brain, too. Studies have shown that often when one lining is weakened, the other is, as well. And people with degenerative brain diseases, like Alzheimer’s, have been found to have large amounts of LPS in their brains. These lipopolysaccharide molecules shouldn’t be there.
Factors that increase gut permeability include:
- Certain medications
- Pathogenic bacteria
 Environmental toxins
Environmental toxins- Elevated blood sugar
- Stress
- Some ingredients like gluten
A third way that our gut bugs help us to stay healthy is by producing important substances for brain health, including BDNF, various vitamins such as B12 and Vitamin K, and neurotransmitters like glutamate and GABA. They also ferment certain food-born compounds like polyphenols, which come from foods like red wine, coffee, and chocolate, into smaller anti-inflammatories so they can be absorbed into the blood stream and, ultimately, protect the brain.
GABA, gamma amino butyric acid, is a neurotransmitter, which means it transmits signals
between brain cells. It’s made by gut bacteria, and its main purpose in the brain is to calm down nerve activity. It normalizes brain waves, and returns the nervous system  to a more stable state. This helps a person deal with stress, which, as we know, causes internal inflammation, among other things. It mutes neuronal activity, and reduces inflammation in the GI tract. There is also research suggesting that because so much GABA is manufactured by bifido bacteria near the bowels, GABA probably plays a role in preventing inflammatory bowel diseases, such as Chron’s disease.
to a more stable state. This helps a person deal with stress, which, as we know, causes internal inflammation, among other things. It mutes neuronal activity, and reduces inflammation in the GI tract. There is also research suggesting that because so much GABA is manufactured by bifido bacteria near the bowels, GABA probably plays a role in preventing inflammatory bowel diseases, such as Chron’s disease.
Another neurotransmitter produced by gut bacteria is glutamate. Glutamate is involved in most aspects of brain activity, including cognition, learning, and memory. Glutamate is abundant in a healthy brain. A whole slew of brain diseases such as anxiety, depression, Alzheimer’s, and attention deficit disorder are associated with a lack of glutamate and GABA.
Something else your gut bugs make is BDNF, brain derived neurotrophic factor. BDNF is responsible for neurogenesis, a process by which new brain cells are made. It also protects existing neurons, and encourages connections, or synapses, between them (and the number of synaptic connections in our brains is linked to how smart we are). There was a study done over decades on older people which showed that the subjects who had less BDNF had twice the risk of developing dementia than those who had higher levels. A lack of BDNF has been noted in patients with all sorts of brain diseases.
In his most recent book, The Grain Brain Whole Life Plan, Perlmutter details some eating habits you can adapt to improve the health of your microbiome. But before getting to that, I want to quickly touch on a factor that comes into play before you have a choice about the foods you send down your gastrointestinal tract. Your birth.
 Humans have evolved over hundreds of thousands of years being birthed out through the birth canal, along with millions of microbes in there. C-sections are messing this up. Researchers have found that babies born via C-section missed out on picking up microbiobial freeloaders on the vaginal highway, which has a profound effect on the infant’s microbiota.
Humans have evolved over hundreds of thousands of years being birthed out through the birth canal, along with millions of microbes in there. C-sections are messing this up. Researchers have found that babies born via C-section missed out on picking up microbiobial freeloaders on the vaginal highway, which has a profound effect on the infant’s microbiota.
A study about the effects of Cesarean section births in the Canadian Medical Association Journal found that this “disruption of the gut microbiota has been linked to an increasing number of diseases, including inflammatory bowel disease, necrotizing enterocolitis, diabetes, obesity, cancer, allergies and asthma.” We wonder why there has been such a rise  in autism, allergies, MS, … maybe messing with our belly bugs has something to do with it. Researchers seem to think so.
in autism, allergies, MS, … maybe messing with our belly bugs has something to do with it. Researchers seem to think so.
The bottom line is – don’t mess with your belly bugs! Think of yourself like Gru, and your gut bugs like your tiny minions inside of you, working hard to keep you and your brain healthy. Take care of them, and they’ll take care of you.
I’ll leave you with these tips on keeping your microbiome healthy from Perlmutter’s latest book, The Grain Brain Whole Life Plan.
- Eat probiotic-rich foods. E.g. Kimchi, live cultured yogurt, and other fermented foods.
- Go low carb and eat high quality fats. Perlmutter recommends looking into a scientifically sound eating protocol consisting of high fats and minimal carbohydrate intake. Lots of good fats like avocados and coconut oil, lots of good fiber from green leafy vegetables like spinach and broccoli, low sugar fruits, lots of nuts, and good proteins like grass-fed beef, lamb, wild fish, and whole eggs.
- Enjoy small amounts of wine, tea, coffee, and chocolate.
 “Small amounts” is the important phrase to bear in mind with this one.
“Small amounts” is the important phrase to bear in mind with this one.
- Eat prebiotics. Food options that are rich in prebiotics are foods like garlic, onion, and leek.
- Drink lots of filtered water. Chlorine, among many other chemicals found in some drinking water, is terrible for your gut. It’s toxic. So get a water filter and enjoy many glasses of clean drinking water.
- Practice intermittent fasting. Perlmutter recommends a type of fasting known as intermittent fasting. Another way to put it would be specific eating windows and specific fasting windows. The fasting windows vary from four hours to eighteen hours. For example fast for twelve hours and eat for twleve hours, or give yourself the option of eating for twelve hours. The logic here is that this type of fasting gives your body adequate time to digest and metabolize your food. During the fasting windows, water is the only thing that’s permitted.